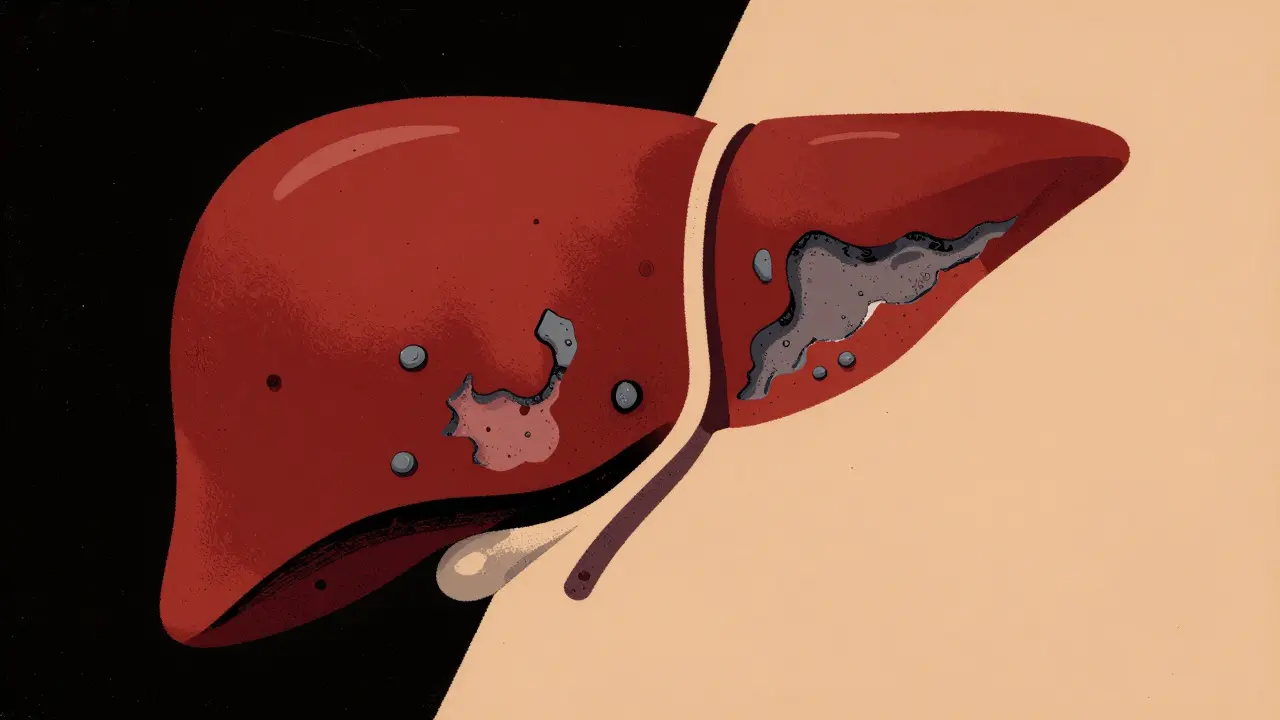
Imagine your liver as a high-efficiency filter for your body. When that filter gets damaged over years of inflammation, it doesn't just stop working-it scars. This process is what we call Cirrhosis is the irreversible end-stage of chronic liver disease where healthy liver tissue is replaced by scar tissue and regenerative nodules. When those scars block blood flow and kill off functioning cells, your body starts to struggle with basic tasks, from filtering toxins to clotting your blood. For many, this starts silently, but once it hits the "decompensated" stage, it becomes a race to manage life-threatening complications.
Key Takeaways
- Cirrhosis is categorized as compensated (no symptoms) or decompensated (overt complications).
- Portal hypertension is the primary driver of dangerous complications like ascites and variceal bleeding.
- MELD and Child-Pugh scores are the gold standards for predicting survival and transplant priority.
- Management focuses on sodium restriction, diuretics, and specific medications like lactulose and rifaximin.
- Biannual ultrasound screening is critical for detecting liver cancer early.
Understanding the Stages: Compensated vs. Decompensated
Not all cirrhosis is the same. In the early stages, you might be "compensated." This means your liver is scarred, but it's still doing enough of the heavy lifting that you don't feel sick. You might just feel a bit more tired than usual, or notice some easy bruising. In fact, about 72% of patients report fatigue early on, often dismissing it as aging or stress.
The real danger arrives when the liver "decompensates." This is the tipping point where the liver can no longer keep up. This transition is a medical red flag. You'll start seeing jaundice-that telltale yellowing of the skin and eyes-because bilirubin levels in the blood climb above 2 mg/dL. This is when the systemic complications start to snowball, affecting your brain, your abdomen, and your blood vessels.
The Scoring Systems: How Doctors Measure Your Risk
Doctors don't just guess how bad the scarring is; they use specific formulas to predict outcomes. The most common is the Child-Pugh-Turcotte system. It looks at five things: bilirubin, albumin, INR (how fast your blood clots), whether you have ascites, and if you're experiencing brain fog. If you're a Class A, your one-year survival rate is nearly 100%. If you're Class C, that number drops to about 45%.
For those needing a transplant, the MELD Score (Model for End-Stage Liver Disease) is the deciding factor. It uses creatinine, bilirubin, and INR to create a numerical value. A score of 15 or higher usually means it's time to start talking about a transplant evaluation. It's a cold, hard number, but it's the fairest way to ensure the sickest people get organs first.
| Feature | Child-Pugh Score | MELD Score |
|---|---|---|
| Primary Use | General prognosis & severity | Transplant prioritization |
| Metrics | Bilirubin, Albumin, INR, Ascites, Encephalopathy | Creatinine, Bilirubin, INR |
| Scale | Class A, B, or C | 6 to 40 (approx) |
| Focus | Liver function & clinical signs | Short-term mortality risk |
Dealing with Portal Hypertension and Ascites
When the liver becomes a mass of scar tissue, blood can't flow through it easily. This creates a backup of pressure in the portal vein, known as Portal Hypertension. Think of it like a traffic jam in your veins. When the pressure gets too high (HVPG ≥10 mmHg), fluid starts leaking into your abdominal cavity. This is Ascites.
Managing this fluid is a constant battle. The first step is almost always a strict sodium diet-usually less than 2 grams a day. That's about one teaspoon of salt for the whole day. Doctors typically prescribe a cocktail of diuretics, like spironolactone and furosemide, to flush the water out. For those who don't respond to meds, a procedure called large-volume paracentesis is used to drain the fluid with a needle. To prevent your blood pressure from crashing during this process, doctors often infuse albumin, which helps keep the remaining fluid in your vessels.
There is a scary side effect here: Spontaneous Bacterial Peritonitis (SBP). This is an infection of the ascitic fluid. Since the fluid is just sitting there, it can become a breeding ground for bacteria. If you develop a fever and abdominal pain, it's an emergency; SBP can have a mortality rate of up to 40% if not treated immediately.
The Danger of Varices and Internal Bleeding
Because the blood can't get through the liver, it looks for detours. It pushes into smaller, fragile veins in the esophagus and stomach. These veins swell up and become Esophageal Varices. The problem is that these veins aren't designed for high pressure. If they pop, the bleeding is massive and life-threatening.
To prevent this, doctors use non-selective beta-blockers like propranolol or nadolol. These meds lower the blood pressure in the portal system, essentially "easing the traffic jam." In some cases, they'll perform an endoscopic band ligation, which is basically like putting tiny rubber bands around the varices to stop them from bleeding. If you're on these meds, you might feel a bit more tired, but it's a trade-off to avoid a catastrophic bleed.
Brain Fog and Hepatic Encephalopathy
Your liver is supposed to clear ammonia from your blood. When it fails, ammonia travels up to your brain, causing Hepatic Encephalopathy. It starts as subtle "brain fog" or irritability and can progress to total confusion or coma. People often describe it as feeling like they're living in a haze.
The go-to treatment is lactulose, a syrup that forces the ammonia out through your bowel movements. The catch? It causes significant diarrhea. Many patients complain that the treatment is as disruptive as the disease, making social outings nearly impossible. For those who keep relapsing, rifaximin-an antibiotic that works in the gut-is added to the mix. This combination can cut hospitalizations by over half.

The Constant Threat: Liver Cancer
A scarred liver is an unstable liver. The constant cycle of damage and attempted repair increases the risk of Hepatocellular Carcinoma (HCC), or primary liver cancer. About 2% to 8% of people with cirrhosis develop this every year. Because early liver cancer doesn't usually cause pain, you can't wait for symptoms.
The standard of care is an ultrasound every six months. While it's not perfect, it's enough to catch tumors at a stage where they can actually be treated. If you're in a screening program, your chances of finding a tumor early are more than double those who aren't being monitored.
Modern Paths to Recovery and Transplantation
While cirrhosis was once seen as a one-way street, new science is offering hope. For those with MASH (metabolic dysfunction-associated steatohepatitis), new drugs like resmetirom are showing that we can actually improve fibrosis in some patients. We're also seeing AI tools like "CirrhoPredict" that can tell a doctor if a patient is likely to decompensate within 90 days, allowing for preemptive care.
When medications aren't enough, a liver transplant is the ultimate solution. It's a grueling process, and the waiting list can be terrifying-about 12% of people don't survive the wait. However, for those who do get the surgery, the transformation is often total. MELD scores plummet, brain fog clears, and people return to full-time work. The key is a multidisciplinary team: a hepatologist, a dietitian for that strict salt diet, and a social worker to navigate the transplant system.
Can cirrhosis be reversed?
Generally, the advanced scarring (fibrosis) of cirrhosis is considered irreversible. However, if the underlying cause-such as alcohol use or hepatitis C-is removed, the liver can stop deteriorating and even improve slightly in function. Some very early stages of fibrosis may regress with new disease-modifying therapies, but true end-stage cirrhosis requires a transplant for a "cure."
What is the most dangerous complication of cirrhosis?
Variceal bleeding is often the most acutely dangerous because it can cause rapid, massive blood loss. However, Hepatic Encephalopathy and SBP (Spontaneous Bacterial Peritonitis) are also high-risk events that can lead to multi-organ failure and death if not managed aggressively.
Why is a low-sodium diet so important for ascites?
Sodium acts like a sponge, holding onto water in your body. In a cirrhotic liver, the body already struggles to regulate fluids and salt. Adding more salt increases the volume of fluid leaking into the abdomen, making ascites worse and rendering diuretics less effective.
How often should I be screened for liver cancer?
Current guidelines from the AASLD recommend an ultrasound every six months for all patients with cirrhosis. This frequency is designed to catch tumors while they are still small enough to be surgically removed or treated with ablation.
Does the MELD score guarantee a transplant?
No, the MELD score is used to prioritize the list, meaning those with higher scores (indicating higher short-term mortality) are generally moved up. However, eligibility also depends on your overall health, support system, and whether you meet specific medical criteria (such as abstinence from alcohol in certain cases).
Next Steps for Patients and Caregivers
If you or a loved one are navigating this, the first priority is finding a specialized hepatologist rather than a general GP. Decompensated cirrhosis requires a level of monitoring that only a specialist can provide. Start a daily log of weight and abdominal girth; a sudden jump in weight usually means fluid is building up before you can even see it.
For those struggling with the side effects of lactulose, talk to your doctor about the timing of doses or adding rifaximin to reduce the frequency of bowel movements. Finally, don't ignore the mental health aspect. The combination of "brain fog" and the stress of a chronic illness is heavy; integrating a social worker or psychologist into your care team can improve medication adherence and overall quality of life.